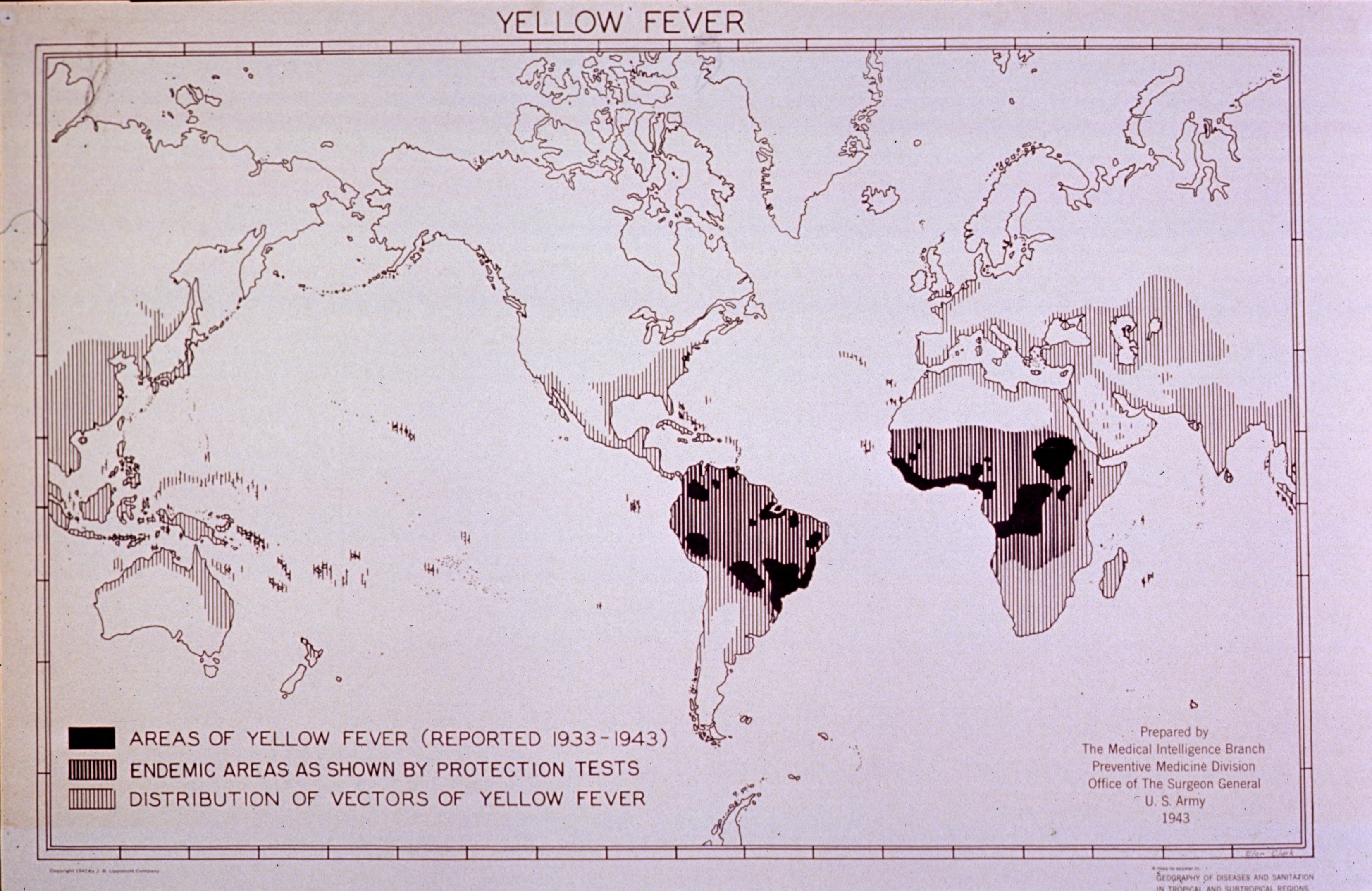
Yellow Fever
Yellow fever had has been around since at least the 18th century and was known and dreaded throughout the 19th century, especially in port towns with the arrival of new ships. It was endemic in Cuba, and so after the Spanish-American War, a Yellow Fever Commission was established in the United States to investigate the disease. Walter Reed was the head of the commission, which established that mosquitoes transmitted the disease. The focus shifted to prevention via mosquito control.
| Dive | ||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||
|
Back in New York, the Rockefeller Institute continued their highly dangerous work on yellow fever. The Rockefeller vaccine was used in the United States and England. At the same time, the Pasteur Institute in Tunis developed a one-dose vaccine (usually combined with smallpox), and it was used in France and their African colonies. The French vaccine was given by scarification (scratching into the skin). It risked febrile and central nervous system reactions but could be done en masson crowds of people at one time.
In 1932, new technique of cultivating the virus in embryonated eggs and freeze drying them came into use. The 17D virus strain from a chance mutation at the Rockefeller Institute was attenuated enough that it didn’t need protective immune serum. Trials continued in South America, but there were problems with encephalitis and jaundice.
| Dive | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||
|
World War II created a huge demand for the yellow fever vaccine. The United States used the Rockefeller Institute vaccine for almost 7 million doses. Later some 26,000 cases of jaundice were recorded and mortality rates of 3 per 1000 (but it was later shown to be Hep. hepatitis B). An investigation ensued. The serum seemed to be the culprit. Serum was donated by those affiliated with the Johns Hopkins' School of Medicine. When the serum was ultimately tested, it was revealed that several of the donors had a history of jaundice.
...